3. As far as maximum safe daily exogenous vitamin D consumption, the numbers seem to be all over the place. Plenty of experts claim the average person should consume at least 10,000 IU daily, with research supporting this. Others put the number far lower.
But apart from perhaps the authors of the South India study, no experts seem concerned that endogenous production of vitamin D in and of itself can reach dangerous levels. The "dissenting opinions" in the UK paper linked in the OP do not mention as a reason for avoiding sun exposure the possibility of toxic or otherwise dangerous levels of vitamin D levels resulting therefrom--rather, they are concerned about increased risk of incidence of skin cancer. Krillin's concern about potential vitamin D toxicity resulting from overexposure to sunlight seems very much a fringe notion. It doesn't have broad, or even narrow, support within the scientific community.
4. What's interesting is that a broad swath of the scientific community is concerned about the potential for exogenous vitamin D supplementation to reach toxic levels with less than 10,000 IU's consumed daily, but they apparently aren't concerned about the potential for endogenous production of vitamin D to reach toxic levels, even though the equilibrium point is about the equivalent of 10,000 IU's daily!
Please, can't we get away from the notion of the average person? Vitamin D should be approached as a hormone, not a vitamin. The required dose for one individual can be toxic for another. Look at this
Vieth paper. In figure 1's middle graph, he gets it right: we have overlapping deficiency and toxicity zones. But that freaks him out so he uses wishful thinking to redraw the graph to have separate deficiency and toxicity zones. It's understandable: more people would be helped than harmed by raising the RDA and UL. But I'm one of the ones who would be harmed. 1000 IU brings me to 45.1 ng/ml. Most papers show a linear relationship between intake and blood levels. I'd be screwed if I listened to him.
A more cunning response to my concern would have been to say, "Thanks for the heads up Krillin. But I test my blood level of vitamin D to make sure I'm getting enough sun, so there's no chance of my getting an overdose."
If the vitamin D3 produced endogenously is indeed identical to the vitamin d3 consumed exogenously, why does the body recognize and regulate levels of the one, but not the other?
Unmetabolized (inactive) vitamin D production is what is regulated in the skin during sunbathing. Then it gets hydroxylated to 25-D. There is little feedback control here. From what I've read, 25-hydroxylation is only inhibited by really high vitamin D activity from both 25-D and 1,25-D. That's how the Marshall Protocol people can have high 1,25 D and low 25-D. Hydroxylation to 1,25 D is tightly controlled by blood calcium level through PTH, unless you're like the Marshall Protocol people who have macrophages going crazy with the 1-hydroxylation.
Thus, the control mechanism is too far upstream for it to work with ingested vitamin D.
6. As far as aging of the skin caused by suinlight goes, I believe most studies have found a significant risk for this only if the skin burns, or at least is exposed unprotected for very long periods of time (2 or more hours on a regular basis). I don't think any study has conclusively shown that exposure without burning, or for less than 1 hour daily, significantly enhances aging of the skin. I believe experts have speculated this may be so, but without conclusive evidence. (If I'm wrong about this, please point me to the appropriate studies.)
Regardless, it's cosmetic. There's an "unholy bargain" a lot of us knowingly strike with a lot of the supplements we take, or things we do to try to stay healthy as long as possible. Often bad comes with the good, and there is an inevitable trade-off that's made. Ex.: I take DHEA. I'm aware of the potential, very slim prostate cancer risk. I still believe the benefits of taking it outweigh the risks.
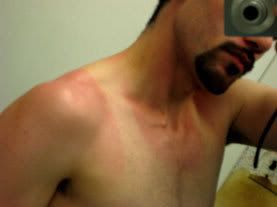
You're just embarrassing yourself here. The inflammatory response begins in a matter of minutes. Ignore inflammation at your peril. Read some articles like these. (erythema = sunburn)
Nature. 1996 Jan 25;379(6563):335-9.
Molecular basis of sun-induced premature skin ageing and retinoid antagonism.
Fisher GJ, Datta SC, Talwar HS, Wang ZQ, Varani J, Kang S, Voorhees JJ.
Department of Dermatology, University of Michigan Medical School, Ann Arbor 48109-0528, USA.
Damage to skin collagen and elastin (extracellular matrix) is the hallmark of long-term exposure to solar ultraviolet irradiation, and is believed to be responsible for the wrinkled appearance of sun-exposed skin. We report here that matrix-degrading metalloproteinase messenger RNAs, proteins and activities are induced in human skin in vivo within hours of exposure to ultraviolet-B irradiation (UVB). Induction of metalloproteinase proteins and activities occurred at UVB doses well below those that cause skin reddening.
Within minutes, low-dose UVB upregulated the transcription factors AP-1 and NF-kappa B, which are known to be stimulators of metalloproteinase genes. All-trans retinoic acid, which transrepresses AP-1 (ref. 8), applied before irradiation with UVB, substantially reduced AP-1 and metalloproteinase induction. We propose that elevated metalloproteinases, resulting from activation of AP-1 and NF-kappa B by low-dose solar irradiation, degrade collagen and elastin in skin. Such damage, if imperfectly repaired, would result in solar scars, which through accumulation from a lifetime of repeated low-dose sunlight exposure could cause premature skin ageing (photoageing).
PMID: 8552187
Acta Dermatovenerol Croat. 2003;11(3):158-62.
Sunscreens--the ultimate cosmetic.
Wolf R, Matz H, Orion E, Lipozencić J.
Dermatology Unit, Kaplan Medical Center, 76100 Rechovot, Israel. wolf_r@netvision.net.il
One decade ago, a sun protection factor (SPF) of 15 was considered a complete blocker of ultraviolet radiation (UV). The logic behind that cutoff point was that sunscreens with this SPF number would always prevent erythema and that preventing erythema would prevent all the ill effects of UV exposure. Today, we know that both of these assumptions were wrong and we tend to recommend higher SPF. Consumers apply only about one-quarter to one-half thickness of the layer of sunscreen material used to measure the SPF in the laboratory. That means that less than 50% of the SPF number claimed on the label is spread on the consumer's skin, meaning that a sunscreen with an SPF 30 will give the real protection of an SPF of 15. Therefore, recommend 60 when you want a real protection of 30!
Significant injury, DNA damage, mutations, and carcinogenesis can and do occur also with cumulative suberythemal UV exposure. Thus, erythema induction, a criterion that defines SPF, is not a good indicator of UV damage. We also need higher SPF values to prevent the damage caused by suberythemal doses of UV. The value of the SPF claimed on the label is diminished by environmental factors that are not taken into account during SPF measurements in the laboratory, such as sweating, water immersion, rubbing off, and photodegradation. There are some misunderstandings and confusion about the mode of action of physical sunscreens. It was originally considered that, in contrast to organic sunscreens, the inorganic metal oxides (zinc oxide and titanium dioxide) acted as scatterers or reflectors of UV light, as a mirror. This is not the case with modern micronized forms of metal oxides. It has been shown that both zinc oxide and titanium dioxide mobilize electrons within their atomic structure while absorbing UV radiation. Thus, although metallic oxides are not inert per se, in their coated form they are stable, non-toxic, and safe and they act as highly efficient UV attenuators. Therefore, we recommend our patients to use this type of sunscreens. We should exert all our influence upon our patients not to expose themselves to excessive sunlight, to routinely use generous layers of sunscreen agents, and to wear protective clothing. To wait for the dust to settle around the issue of the effectiveness of sunscreens in preventing melanoma, while the ideal sunscreens--topical, systemic, whatever--are at our disposal, is a luxury we cannot afford.
PMID: 12967508